Rashes: Symptoms, Causes, Types, Diagnosis, and Treatments
Rashes are among the most common skin problems encountered by people of all ages worldwide. Although often harmless, they can sometimes indicate underlying health issues that require prompt medical attention. Understanding rashes — their symptoms, causes, types, diagnosis, and treatment options — empowers individuals to manage their skin health effectively.
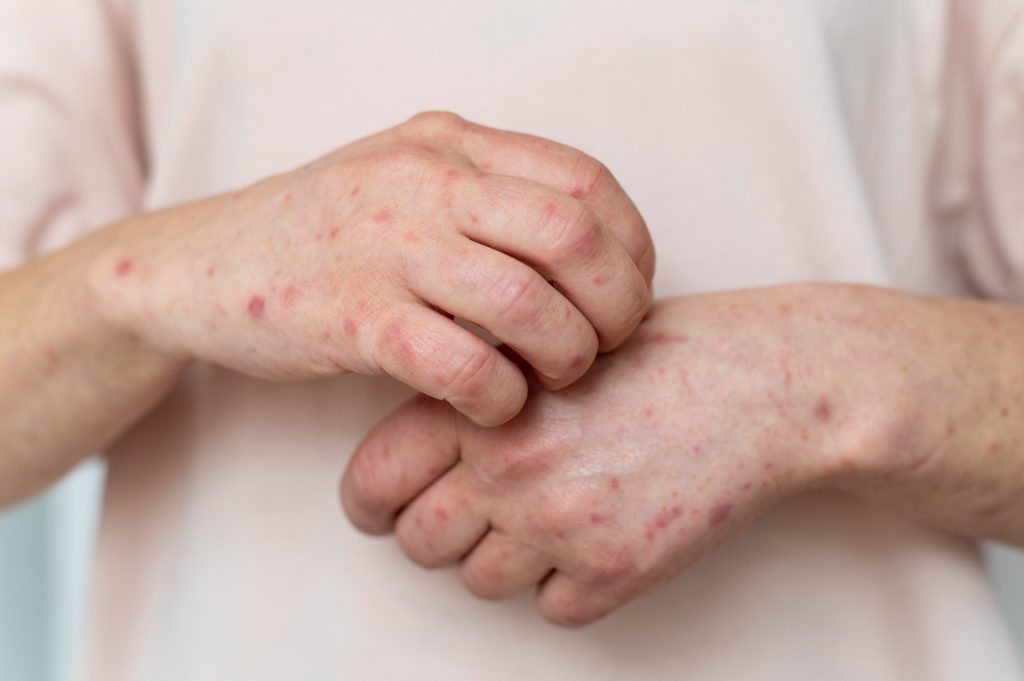
What is a Rash?
A rash is an area of irritated or swollen skin that can appear anywhere on the body. Rashes may look like red spots, bumps, blisters, scales, or patches and can cause itching, pain, dryness, or swelling. While many rashes resolve on their own, some require medical evaluation to avoid complications.
Symptoms of Rashes
Rashes manifest differently depending on their cause and type. Common symptoms include:
- Redness: The skin appears flushed or inflamed.
- Itching (Pruritus): An urge to scratch the affected area.
- Bumps or Blisters: Raised areas that may be filled with fluid.
- Scaling or Flaking: Peeling or shedding of the outer skin layer.
- Swelling: Puffiness or raised areas due to inflammation.
- Pain or Burning: Some rashes cause discomfort or a stinging sensation.
- Dryness or Cracking: The skin may become rough or fissured.
- Warmth: The affected skin may feel warmer than surrounding areas.
- Oozing or Crusting: Fluid may leak from blisters and dry up forming crusts.
When to see a doctor:
Seek medical advice if the rash is accompanied by fever, difficulty breathing, swelling of the face or lips, rapid spreading, severe pain, or signs of infection like pus.
Causes of Rashes
Rashes arise due to a wide array of causes, broadly categorized into:
1. Allergic Reactions
Allergic contact dermatitis is triggered by direct skin contact with allergens such as:
- Poison ivy, poison oak
- Nickel or other metals in jewelry
- Fragrances, cosmetics
- Latex
- Certain medications
2. Infections
Skin infections caused by bacteria, viruses, fungi, or parasites can result in rashes:
- Bacterial: Impetigo, cellulitis
- Viral: Chickenpox, measles, shingles
- Fungal: Ringworm, candidiasis
- Parasitic: Scabies, lice infestations
3. Chronic Skin Conditions
Persistent skin disorders that cause rashes include:
- Eczema (Atopic dermatitis)
- Psoriasis
- Rosacea
- Seborrheic dermatitis
4. Environmental Factors
Exposure to irritants or extreme conditions can provoke rashes:
- Sunburn
- Heat rash (miliaria) from sweat blockage
- Contact with harsh chemicals or detergents
5. Systemic Diseases
Certain internal illnesses manifest as skin rashes:
- Lupus erythematosus
- Dermatomyositis
- Kawasaki disease
- Lyme disease
6. Medications and Drugs
Adverse drug reactions can cause drug-induced rashes, often appearing as:
- Maculopapular eruptions
- Urticaria (hives)
- Stevens-Johnson syndrome (severe)
Types of Rashes
Rashes are classified based on their appearance, pattern, and cause. Understanding the type aids in diagnosis and treatment.
1. Macular Rash
Flat, red spots (macules) appear on the skin, such as in measles or scarlet fever.
2. Papular Rash
Raised bumps (papules) that can be felt, often seen in eczema or insect bites.
3. Maculopapular Rash
Combination of flat and raised red areas common in viral infections like rubella.
4. Vesicular Rash
Small fluid-filled blisters (vesicles), as seen in chickenpox and shingles.
5. Pustular Rash
Pus-filled bumps (pustules), characteristic of acne or impetigo.
6. Urticarial Rash (Hives)
Raised, itchy welts that may vary in size, commonly due to allergies.
7. Erythematous Rash
Redness caused by increased blood flow in the skin, common in infections or inflammation.
8. Petechial or Purpuric Rash
Small pinpoint red or purple spots caused by bleeding under the skin, often requiring urgent care.
9. Scaly Rash
Rough, flaky skin seen in psoriasis and seborrheic dermatitis.
10. Lichenified Rash
Thickened, leathery skin from chronic scratching, typical in chronic eczema.
Diagnosis of Rashes
Diagnosing a rash involves a combination of clinical examination, history-taking, and sometimes laboratory tests.
1. Medical History
Your doctor will ask about:
- Onset and duration of rash
- Associated symptoms like itching, fever
- Recent exposures (new soaps, medications, travel, insect bites)
- Past skin problems or allergies
- Family history of skin diseases
2. Physical Examination
Inspection of rash characteristics:
- Location and distribution
- Morphology (shape, size, color)
- Presence of secondary changes (crusting, scaling)
- Associated lymph node enlargement or systemic signs
3. Laboratory Tests
To identify infectious or autoimmune causes:
- Skin biopsy: Small sample examined under microscope.
- Blood tests: To check for infections, autoimmune markers, or allergies.
- Patch testing: Identifies contact allergens.
- Skin scrapings: For fungal or parasitic infections.
- Culture tests: For bacterial or viral pathogens.
4. Imaging and Other Tests
Rarely, imaging may be needed if systemic involvement is suspected.
Treatments for Rashes
Treatment depends on the underlying cause, type, and severity of the rash. Some rashes resolve spontaneously, while others require targeted therapy.
1. General Measures
- Avoid irritants: Identify and stop exposure to allergens or harsh chemicals.
- Keep skin clean and dry: Gentle cleansing with mild soap.
- Moisturize: Use hypoallergenic emollients to prevent dryness.
- Avoid scratching: Use cold compresses and keep nails trimmed.
2. Medications
a. Topical Treatments
- Corticosteroids: Reduce inflammation and itching (hydrocortisone, betamethasone). Use under medical guidance.
- Antihistamines: Oral or topical to relieve itching in allergic rashes.
- Antibiotics/Antifungals: For bacterial or fungal infections (mupirocin, clotrimazole).
- Calcineurin inhibitors: Tacrolimus or pimecrolimus for eczema.
- Moisturizers with ceramides: Restore skin barrier function.
b. Systemic Treatments
- Oral corticosteroids: For severe inflammatory rashes.
- Antibiotics/Antivirals: For infections like cellulitis or shingles.
- Immunosuppressants: Methotrexate, cyclosporine for chronic autoimmune rashes.
- Biologics: Targeted therapies for psoriasis or atopic dermatitis.
3. Phototherapy
Controlled exposure to ultraviolet light benefits some chronic rashes like psoriasis.
4. Home Remedies
- Oatmeal baths: Soothe itching and irritation.
- Aloe vera gel: Natural anti-inflammatory.
- Cold compresses: Relieve swelling and itching.
Preventing Rashes
While not all rashes can be prevented, you can reduce your risk by:
- Using gentle, fragrance-free skincare products.
- Avoiding known allergens and irritants.
- Wearing protective clothing outdoors.
- Maintaining good hygiene and skin care routines.
- Managing chronic skin conditions under medical supervision.
- Keeping your environment clean to reduce exposure to infectious agents.
When to Seek Immediate Medical Attention
Certain rash presentations require urgent care, including:
- Rapidly spreading rash with fever (possible meningitis or sepsis)
- Rash accompanied by difficulty breathing or swelling (anaphylaxis)
- Painful blistering or peeling skin (Stevens-Johnson syndrome)
- Purplish spots or bruises without injury (possible bleeding disorder)
- Rash with neurological symptoms or joint pain
Conclusion
Rashes are a frequent and sometimes alarming skin condition with a wide range of causes and presentations. Recognizing symptoms, understanding potential causes, knowing when to seek medical care, and following appropriate treatment protocols are key to effective management. If you develop a persistent, worsening, or unexplained rash, consulting a healthcare professional ensures accurate diagnosis and timely treatment, safeguarding your skin health and overall well-being.
Frequently Asked Questions (FAQs) About Rashes
What causes a rash to appear suddenly?
Sudden rashes often result from allergic reactions, infections, or contact with irritants like poison ivy or chemicals. Identifying the trigger helps in timely treatment.
How can I tell if a rash is serious?
A rash accompanied by fever, swelling, difficulty breathing, spreading rapidly, or painful blisters may indicate a serious condition and requires immediate medical attention.
Can stress cause rashes?
Yes, stress can trigger or worsen certain skin conditions like eczema, psoriasis, and hives, leading to the development or aggravation of rashes.
Are all rashes itchy?
Not all rashes cause itching. Some may be painless or cause burning, scaling, or redness without itchiness, depending on the cause.
How long does a typical rash last?
The duration varies; some rashes clear within a few days (like heat rash), while chronic rashes (eczema or psoriasis) may persist for weeks or months without proper treatment.
Can rashes be contagious?
Certain rashes caused by infections (chickenpox, ringworm, impetigo) are contagious, while others like eczema or allergic dermatitis are not.
What are the best home remedies for mild rashes?
For mild rashes, soothing oatmeal baths, cold compresses, gentle moisturizing, and avoiding irritants can help relieve symptoms.
When should I see a dermatologist for a rash?
Consult a dermatologist if the rash persists longer than two weeks, worsens despite treatment, or recurs frequently.
Can medications cause rashes?
Yes, many medications can trigger allergic or drug-induced rashes. Always inform your doctor about any new skin changes after starting medication.
How are rashes diagnosed by doctors?
Doctors use medical history, physical exams, skin biopsies, patch tests, and lab tests to identify the cause and type of rash accurately.
Are there different types of rashes for children and adults?
While many rashes affect all ages, some are more common in children (like chickenpox) or adults (like shingles), and treatment approaches may differ accordingly.
Is sun exposure harmful to someone with a rash?
Sun exposure can worsen certain rashes, such as lupus or photosensitive eczema, but in some cases, controlled phototherapy is used therapeutically under medical supervision.
Can dietary changes help in managing rashes?
For some individuals, avoiding allergens or inflammatory foods may reduce rash flare-ups, especially in conditions like eczema or psoriasis.
How do I prevent rashes caused by allergic reactions?
Avoid known allergens, use hypoallergenic skincare products, wear protective clothing, and perform patch testing if necessary to prevent allergic rashes.
Are there permanent treatments for chronic rashes?
While some chronic rashes cannot be permanently cured, ongoing treatment and lifestyle adjustments can manage symptoms and reduce flare-ups effectively.
For more details keep visiting our Website & Facebook Page.
